What is Meningitis?
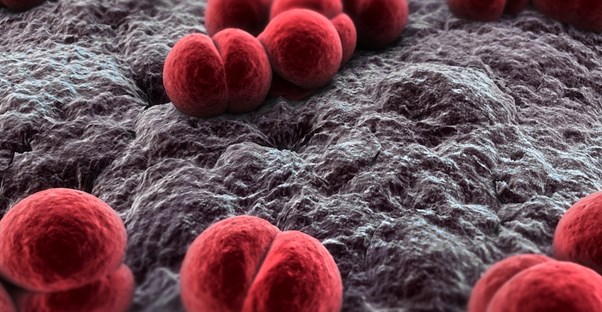
Meningococcal disease is a collection of illnesses caused by Neisseria meningitidis, most commonly leading to meningitis, or bacterial meningitis. When a person is infected, the protective membranes covering the brain and spinal cord (meninges) begin to swell, characterized by sudden fever, headache, and stiffness of the neck.
Approximately 10-15% of meningococcal disease cases are fatal, and up to 20% of patients who recover experience long term disabilities, such as loss of limbs, deafness, brain damage, and problems with the nervous system.
Symptoms of meningitis may develop over several hours or days, and early symptoms may mimic the flu. Possible signs of a meningitis infection include: sudden high fever, stiff neck, severe headache, nausea, vomiting, confusion, difficulty concentrating, seizures, fatigue, difficulty waking, sensitivity to light, lack of appetite or thirst, and/or skin rash.
Meningitis-causing bacteria hides in the back of the nose and throat, sometimes without any indication of illness, and is spread from person to person through infected respiratory droplets. However, the bacteria cannot be passed through casual contact or sharing air with an infected person.
Although most cases in the U.S. are caused by viral infection, meningitis can also present as bacterial meningitis, fungal meningitis, parasitic meningitis, amebic meningitis, and non-infectious meningitis. Because bacterial meningitis can be fatal without prompt treatment, seek medical attention if you experience symptoms of meningitis.
What types of meningococcal vaccines are there?
Meningococcal Conjugate Vaccines
Conjugate vaccines refer to a specific method of vaccination, in which a protein is joined to part of the target bacteria to improve the body’s immune response. The two meningococcal conjugate vaccines currently on the market are Menactra and Menveo. Both are given in two separate doses to preteens, teens, and people at increased risk for meningococcal disease. These vaccines protect against serogroups A, C, W, and Y.
Serogroup B (Recombinant) Meningococcal Vaccines
Unlike conjugate vaccines, recombinant vaccines use existing proteins from certain bacteria to help the body build protection. The two recombinant meningococcal vaccines on the market are Bexsero and Trumenba, and protect only against serogroup B. These vaccines are administered in two doses to people between the ages of 16 and 23 who are at average risk of catching meningococcal disease, as well as those between the ages of 10 and 16 who are at an increased risk.
Who should receive the vaccine and when?
The Centers for Disease Control and Prevention (CDC) recommends that all preteens age 11-12 receive the meningococcal conjugate vaccine, with a booster dose at age 16. In addition, teens and young adults (16-23 years old) may also be vaccinated with a serogroup B meningococcal vaccine. The ideal time for the second vaccine is between the ages of 16 and 18.
For teens who suffer from Complement Component Deficiency, are prescribed Soliris, have suffered spleen damage or removal, or are identified to be at increased risk because of an outbreak, the CDC recommends the second vaccine more strongly.
Additionally, babies who suffer from Complement Component Deficiency, are prescribed Soliris, have suffered spleen damage or removal, have HIV, are traveling or residing in countries where the disease is common, or are identified to be at increased risk because of an outbreak should receive a meningococcal conjugate vaccine between 2 months and 10 years old.
Seek medical attention before receiving the meningococcal vaccine if you or your child has had a life-threatening allergic reaction to any of these vaccines, are not feeling well at the scheduled time of injection, or if you are pregnant or breastfeeding.
Are there any side effects?
Vaccines, like any medicine, come with the risk of side effects, although most of the time people immunized with a meningococcal vaccine do not experience any serious problems. In cases where reactions occur, most are mild and subside within a few days.
Mild reactions from meningococcal conjugate vaccines include soreness and redness at the injection site, as well as fever. After receiving serogroup b meningococcal vaccines, people have documented soreness, redness, and swelling at the injection site, in addition to fatigue, headaches, muscle or joint pain, fever, nausea, and diarrhea.
What injuries are associated with the vaccine?
In some cases, symptoms persist and develop into something more serious. Injuries that have been associated with the meningococcal conjugate vaccine include:
- Acute Disseminated Encephalomyelitis (ADEM)
- Guillain-Barré Syndrome (GBS)
- Idiopathic Thrombocytopenic Purpura (ITP)
- Multiple Sclerosis (MS)
- Transverse Myelitis (TM)
If the resulting injury lasts more than 6 months, results in surgical intervention during inpatient hospitalization, or results in death, you may be eligible to petition for compensation through the National Vaccine Injury Compensation Program.
National Vaccine Injury Compensation Program
Vaccines are an important part of public health, working to save lives by preventing disease. Most of the time, vaccines are administered without any serious problems. Like with any medication, however, there is a risk of side effects, ranging from mild to serious.
For this reason, the US government created the National Vaccine Injury Compensation Program (NVICP), a “no-fault” alternative to the traditional legal system. Petitions can be filed by any individual, at any age, after developing an injury believed to be a result of a covered vaccine, if jurisdictional requirements are met.
Conway Homer, P.C. is the most experienced vaccine injury law firm in the United States. We represent clients from all 50 states and have advocated for landmark cases that have shaped the Vaccine Program and made it friendlier and more generous to individuals who suffer from vaccine injuries. To get in touch with our dedicated team, click here for a free consultation.